The Silent Siege: Coronary Artery Disease – An Epic of Prevention and Management
The human heart, a marvel of biological engineering, beats tirelessly, an unwavering engine driving life itself. Yet, even this most resilient of organs is susceptible to a silent, insidious siege: Coronary Artery Disease (CAD). More than just a medical condition, CAD is a narrative – a complex story woven from genetics and lifestyle, environmental factors and personal choices, scientific breakthroughs and the unwavering human spirit. It is the leading cause of death worldwide, a stark reminder of our vulnerability, but also a testament to the power of knowledge, prevention, and proactive management. For the knowledgeable reader, understanding CAD is not merely about reciting facts, but about comprehending a profound biological drama, one in which each of us plays a role.
This is the story of that battle: from the microscopic origins of plaque to the grand strategies of public health, from the quiet discipline of daily habits to the cutting-edge interventions of modern medicine. It is a story that demands our attention, for within its unfolding lies the blueprint for a healthier, more vibrant future.
Chapter 1: The Genesis of a Silent Threat – Understanding Atherosclerosis
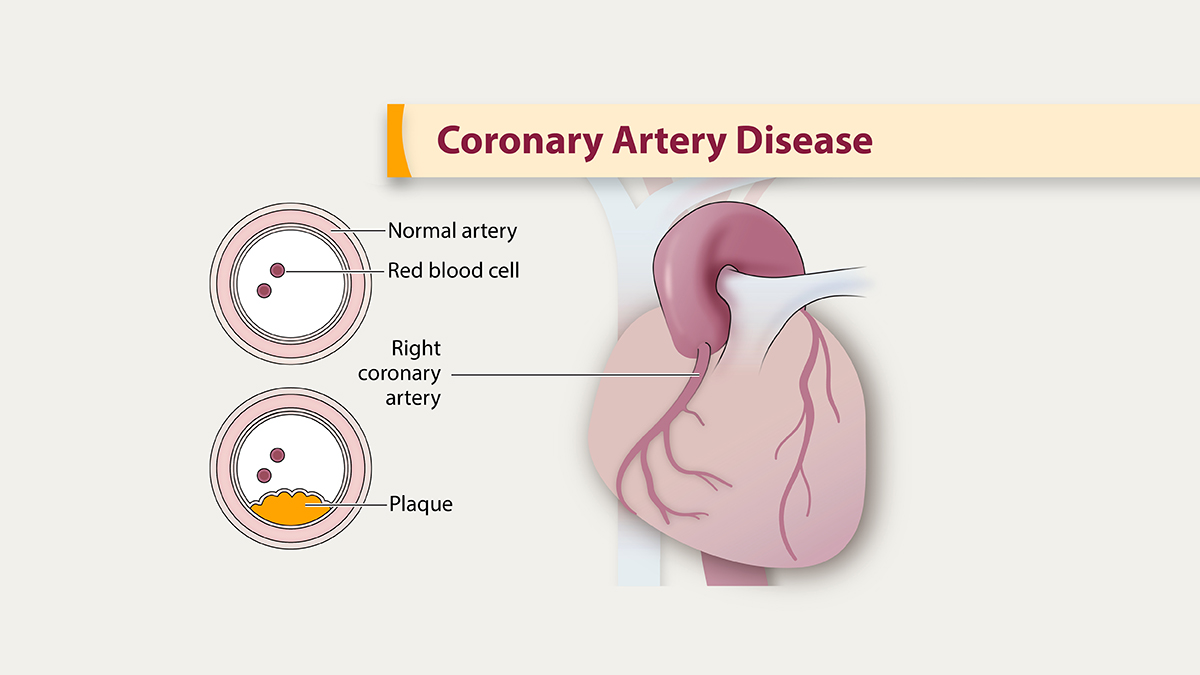
The narrative of CAD begins not with a dramatic event, but with a slow, almost imperceptible process known as atherosclerosis. Imagine the coronary arteries – the vital blood vessels supplying the heart muscle itself – as pristine, smooth-walled conduits. Atherosclerosis is the gradual hardening and narrowing of these arteries due to the buildup of a sticky substance called plaque. This plaque, a complex concoction of cholesterol, fatty substances, calcium, and inflammatory cells, begins its insidious creep often in early adulthood, silently gathering momentum over decades.
The genesis of this plaque is a tale of endothelial dysfunction. The endothelium, the delicate inner lining of blood vessels, acts as a protective barrier and regulator of vascular tone. Damage to this lining, often initiated by factors like high blood pressure, elevated LDL (low-density lipoprotein) cholesterol, smoking, and high blood sugar, creates microscopic breaches. Through these breaches, LDL particles infiltrate the arterial wall, where they become oxidized. This oxidized LDL is a powerful inflammatory signal, attracting monocytes – a type of white blood cell – which then transform into macrophages. These macrophages gorge themselves on the oxidized LDL, becoming "foam cells," the earliest visible components of atherosclerotic plaque.
As more foam cells accumulate, along with smooth muscle cells migrating from the vessel wall and connective tissue, the plaque grows. Initially, this growth might be "outward" (positive remodeling), not significantly impeding blood flow. But eventually, it protrudes into the vessel lumen, narrowing the artery and restricting the supply of oxygen-rich blood to the heart muscle – a condition known as myocardial ischemia. This is when symptoms like angina (chest pain or discomfort) may begin to manifest, often during physical exertion when the heart's demand for oxygen outstrips its supply.
The true danger, however, often lies in the instability of the plaque. Some plaques are "vulnerable," characterized by a thin fibrous cap separating the lipid-rich core from the bloodstream. When this cap ruptures, it exposes the highly thrombogenic (clot-forming) contents of the plaque to the blood. This triggers a rapid cascade of events: platelets rush to the site, forming a blood clot (thrombus) that can quickly and completely occlude the artery. This sudden blockage is the cause of a myocardial infarction, or heart attack, where a portion of the heart muscle dies due to lack of blood supply. If the blockage is not cleared quickly, it can lead to irreversible damage, heart failure, or even sudden cardiac death.
Understanding this pathophysiological narrative is the first essential step. It reveals that CAD is not merely a disease of old age, but a lifelong process influenced by a multitude of factors, some within our control, others less so.
Chapter 2: The Modifiable and Unmodifiable – Risk Factors in the CAD Story
Every story has its protagonists and antagonists. In the CAD narrative, risk factors are the forces shaping the plot. Some are unchangeable – the hand we're dealt – while others offer opportunities for intervention and rewrite the ending.
The Unmodifiable Chapters:
- Age: The older we get, the higher the risk. Atherosclerosis is a progressive process.
- Sex: Historically, men have a higher risk at younger ages. Women's risk increases significantly after menopause, often catching up to men's in later life.
- Family History/Genetics: A strong family history of early CAD (e.g., father or brother before age 55, mother or sister before age 65) indicates a genetic predisposition. This isn't a destiny sentence but a crucial alert to be more vigilant about modifiable risks.
The Modifiable Chapters – Where Agency Takes Hold:
These are the elements of the story where our choices and actions become paramount.
- High Blood Pressure (Hypertension): The "silent killer." Sustained high pressure damages the endothelial lining, accelerating plaque formation and increasing the risk of plaque rupture. It's a constant stressor on the arterial walls.
- High Cholesterol (Dyslipidemia): Specifically, high LDL cholesterol is a primary driver of atherosclerosis. LDL transports cholesterol into arterial walls. Conversely, high HDL (high-density lipoprotein) cholesterol, which helps remove cholesterol from the arteries, is generally protective. High triglycerides also contribute to risk.
- Diabetes Mellitus: Both type 1 and type 2 diabetes significantly increase CAD risk. High blood glucose levels damage blood vessels, accelerate atherosclerosis, and contribute to other risk factors like dyslipidemia and hypertension. Diabetes is often considered a "CAD equivalent," meaning the risk of a heart attack in a diabetic patient is similar to someone who has already had one.
- Smoking: Perhaps the single most potent and preventable risk factor. Nicotine and thousands of other toxins in tobacco smoke directly damage the endothelium, promote inflammation, reduce HDL, increase blood clotting tendency, and cause vasoconstriction. Quitting smoking is the most impactful step an individual can take to reduce their CAD risk, with benefits seen almost immediately.
- Obesity: Especially central adiposity (fat around the waist), is closely linked to insulin resistance, inflammation, hypertension, and dyslipidemia – a constellation of risks often termed "metabolic syndrome."
- Physical Inactivity (Sedentary Lifestyle): A lack of regular physical activity contributes to obesity, hypertension, diabetes, and unfavorable lipid profiles. Exercise is a powerful anti-inflammatory and cardiovascular tonic.
- Unhealthy Diet: Diets high in saturated and trans fats, refined carbohydrates, added sugars, and sodium, and low in fruits, vegetables, whole grains, and lean proteins, directly fuel dyslipidemia, inflammation, and metabolic dysfunction.
- Psychosocial Factors (Stress, Depression, Anxiety): Chronic psychological stress triggers physiological responses (e.g., elevated cortisol, increased heart rate and blood pressure) that can contribute to endothelial dysfunction and inflammation. Depression and anxiety are increasingly recognized as independent risk factors and can also negatively impact adherence to healthy lifestyle changes.
- Sleep Apnea: Untreated sleep apnea, characterized by interrupted breathing during sleep, leads to intermittent hypoxia and surges in blood pressure, significantly increasing CAD risk.
- Air Pollution: Emerging research highlights ambient air pollution as a contributor to cardiovascular disease, inducing systemic inflammation and oxidative stress.
Recognizing these characters in the CAD story empowers individuals to become active participants in shaping their health destiny.
Chapter 3: The Art of Prevention – Building a Resilient Fortress
The most compelling chapter in the CAD story is prevention. It is here that we move from understanding the threat to actively constructing a defense. Primary prevention aims to prevent CAD from ever developing, while secondary prevention focuses on preventing further events in those already diagnosed. The strategies, however, are largely the same, differing only in intensity and urgency.
The Cornerstone: Lifestyle Interventions
Lifestyle is not merely a recommendation; it is the bedrock of prevention and management.
Dietary Discipline: The Plate as a Prescription.
- Mediterranean Diet: Often hailed as the gold standard. Emphasizes fruits, vegetables, whole grains, legumes, nuts, seeds, olive oil as the primary fat source, fish, and moderate consumption of poultry, dairy, and red wine, with minimal red meat and processed foods. Its anti-inflammatory and antioxidant properties are profound.
- DASH Diet (Dietary Approaches to Stop Hypertension): Focuses on reducing sodium intake, and increasing potassium, calcium, and magnesium through fruits, vegetables, whole grains, and low-fat dairy. Highly effective for blood pressure control.
- Plant-Based Diets: Emphasize whole, unprocessed plant foods. Can be highly effective in lowering cholesterol, blood pressure, and blood sugar.
- Key Principles:
- Limit Saturated and Trans Fats: Found in red meat, processed foods, fried foods, and some dairy. Opt for monounsaturated (olive oil, avocados, nuts) and polyunsaturated fats (fatty fish, flaxseed, walnuts).
- Reduce Sodium Intake: Processed foods are major culprits. Aim for less than 2,300 mg/day, ideally closer to 1,500 mg/day for those with hypertension or high risk.
- Minimize Added Sugars: Found in sugary drinks, desserts, and many processed foods. Contribute to inflammation, weight gain, and dyslipidemia.
- Increase Fiber: Found in fruits, vegetables, whole grains, and legumes. Soluble fiber helps lower LDL cholesterol.
- Lean Protein Sources: Fish, poultry, legumes, tofu.
- Portion Control: Even healthy foods, in excess, can lead to weight gain.
Physical Activity: Movement as Medicine.
- Aerobic Exercise: At least 150 minutes of moderate-intensity (brisk walking, swimming, cycling) or 75 minutes of vigorous-intensity (running, high-impact aerobics) exercise per week.
- Strength Training: At least two days a week, working all major muscle groups. Builds muscle mass, which boosts metabolism and improves glucose utilization.
- Beyond Structured Exercise: Minimize sedentary time. Incorporate movement throughout the day – standing desks, walking breaks, taking stairs. Exercise improves endothelial function, lowers blood pressure, reduces LDL, increases HDL, and helps manage weight and blood sugar.
Weight Management: Balancing the Scales.
- Achieving and maintaining a healthy weight (BMI between 18.5 and 24.9 kg/m²) is crucial. For those overweight or obese, even a modest weight loss (5-10% of body weight) can significantly improve risk factors. Focus on sustainable changes in diet and exercise rather than fad diets. Waist circumference (ideally <40 inches for men, <35 inches for women) is also a key indicator of central adiposity and metabolic risk.
Smoking Cessation: Extinguishing the Fire.
- The single most impactful preventive measure. Quitting smoking dramatically reduces CAD risk within months, with risk continuing to decline over years, eventually approaching that of a non-smoker. Utilize nicotine replacement therapy, medications (e.g., bupropion, varenicline), and counseling support.
Stress Management and Mental Well-being: Nurturing the Mind-Heart Connection.
- Chronic stress can impact cardiovascular health. Techniques like mindfulness meditation, yoga, deep breathing exercises, spending time in nature, engaging in hobbies, and maintaining strong social connections can mitigate stress. Addressing underlying depression and anxiety with professional help is equally vital.
Optimal Sleep: The Restorative Power.
- Aim for 7-9 hours of quality sleep per night. Poor sleep hygiene, chronic sleep deprivation, and sleep disorders like sleep apnea contribute to hypertension, insulin resistance, and inflammation.
The Medical Armory: Pharmacological Prevention
For individuals with elevated risk factors, lifestyle changes may be augmented by pharmacotherapy, especially in primary prevention.
- Statins: These HMG-CoA reductase inhibitors are highly effective in lowering LDL cholesterol and have pleiotropic effects, including plaque stabilization and anti-inflammatory properties. They are often prescribed based on individual risk assessment (e.g., ASCVD risk calculator).
- Antihypertensives: A variety of medications (e.g., ACE inhibitors, ARBs, beta-blockers, calcium channel blockers, diuretics) are available to control high blood pressure, thereby reducing endothelial stress.
- Antiplatelet Therapy (Aspirin): While once widely recommended for primary prevention, the role of daily low-dose aspirin has been refined. It is now generally reserved for individuals with a high ASCVD risk who do not have an increased bleeding risk, and typically after shared decision-making with a physician. Its benefit for primary prevention is not universal and must be carefully weighed against the risk of bleeding.
- Diabetes Medications: Beyond lifestyle, medications like metformin, GLP-1 receptor agonists, and SGLT2 inhibitors not only control blood sugar but have demonstrated significant cardiovascular benefits.
Prevention is a proactive narrative, a commitment to daily choices that build resilience and safeguard the heart.
Chapter 4: Navigating the Waters – Management After Diagnosis
When CAD has already established its presence, the story shifts from primary prevention to comprehensive management. The goal now is to prevent disease progression, avert acute events, alleviate symptoms, and improve quality of life and longevity. This chapter involves a multi-pronged approach combining intensified lifestyle changes, advanced pharmacotherapy, and, when necessary, interventional or surgical procedures.
The Medical Arsenal: Advanced Pharmacotherapy (Secondary Prevention)
For those with established CAD, medication is a cornerstone of management, often lifelong.
- Antiplatelet Agents:
- Aspirin: Typically prescribed indefinitely for most CAD patients to prevent clot formation.
- P2Y12 Inhibitors (e.g., clopidogrel, ticagrelor, prasugrel): Often prescribed in combination with aspirin (dual antiplatelet therapy, DAPT) after an acute coronary syndrome (ACS) or coronary stenting, for a specified duration to prevent stent thrombosis and recurrent ischemic events.
- High-Intensity Statins: Essential for stabilizing plaque, lowering LDL, and reducing the risk of future events. Doses are often higher than for primary prevention.
- Beta-Blockers: Prescribed after a heart attack or for those with heart failure, they reduce myocardial oxygen demand by slowing heart rate and reducing contractility. They also help control blood pressure and reduce the risk of arrhythmias.
- ACE Inhibitors or Angiotensin Receptor Blockers (ARBs): Particularly beneficial for patients with hypertension, diabetes, heart failure, or impaired left ventricular function post-MI. They reduce blood pressure, improve endothelial function, and help remodel the heart.
- Nitrates (e.g., nitroglycerin): Used to relieve angina symptoms by dilating coronary arteries and reducing cardiac workload. Can be short-acting (sublingual) for acute relief or long-acting (patches, oral forms) for prevention of symptoms.
- Newer Agents with Cardiovascular Benefits:
- PCSK9 Inhibitors (e.g., evolocumab, alirocumab): Powerful injectable drugs for dramatically lowering LDL cholesterol, often used in patients with very high risk or those who cannot achieve target LDL levels with statins alone.
- SGLT2 Inhibitors (e.g., empagliflozin, dapagliflozin): Originally for diabetes, these oral medications have shown remarkable cardiovascular and renal benefits, particularly in patients with heart failure and kidney disease, regardless of diabetes status.
- GLP-1 Receptor Agonists (e.g., liraglutide, semaglutide): Also diabetes medications, they have demonstrated significant cardiovascular risk reduction and weight loss benefits.
- Colchicine: An anti-inflammatory drug being explored for its role in reducing recurrent cardiovascular events in patients with established CAD, targeting the inflammatory component of atherosclerosis.
The Interventional and Surgical Chapters
When medication and lifestyle are insufficient to manage symptoms or prevent acute events, more direct interventions may be required.
- Percutaneous Coronary Intervention (PCI) / Angioplasty and Stenting:
- A minimally invasive procedure where a catheter is threaded through a blood vessel (usually in the wrist or groin) to the heart. A balloon is inflated at the site of a blockage to open the artery, and then a small mesh tube (stent) is usually deployed to keep the artery open. Drug-eluting stents, which slowly release medication to prevent restenosis, are now standard. PCI is often performed urgently during a heart attack (primary PCI) to restore blood flow quickly and limit heart muscle damage.
- Coronary Artery Bypass Grafting (CABG):
- A major open-heart surgical procedure. A healthy blood vessel (often from the leg, arm, or chest wall) is harvested and grafted to bypass the blocked section of the coronary artery, creating a new pathway for blood flow to the heart muscle. CABG is typically considered for patients with multiple severe blockages, left main coronary artery disease, or complex anatomy not amenable to stenting, especially in those with diabetes or impaired heart function.
The choice between PCI and CABG is complex, based on the number and location of blockages, overall heart function, patient comorbidities, and shared decision-making between the patient and a multidisciplinary heart team.
The Unsung Hero: Cardiac Rehabilitation
Cardiac rehabilitation (CR) is a structured, medically supervised program designed to help patients recover from a heart attack, heart surgery, or other forms of heart disease. It's a crucial, yet often underutilized, chapter in the management story.
- Supervised Exercise Training: Tailored exercise programs to improve cardiovascular fitness, strength, and endurance, while ensuring safety.
- Education: Comprehensive education on heart-healthy living, including diet, exercise, medication adherence, and risk factor modification.
- Psychosocial Support: Addressing the emotional toll of heart disease, including anxiety, depression, and stress, often through counseling and support groups.
- Risk Factor Modification: Intensive management of blood pressure, cholesterol, diabetes, and smoking cessation.
CR has been shown to significantly reduce mortality, improve quality of life, and reduce the likelihood of future cardiac events. It empowers patients to take an active role in their long-term recovery and well-being.
The Lifelong Narrative: Self-Management and Shared Decision-Making
Living with CAD is a lifelong journey, a continuous narrative of self-management and partnership with healthcare providers. This involves:
- Strict Adherence to Medications: Understanding the purpose and importance of each drug.
- Ongoing Lifestyle Commitment: The healthy habits cultivated for prevention remain crucial for management.
- Regular Follow-ups: Consistent monitoring of blood pressure, cholesterol, blood sugar, and overall heart function.
- Symptom Awareness: Recognizing and promptly reporting any new or worsening symptoms.
- Psychological Resilience: Seeking support for the emotional and psychological challenges of chronic illness.
- Shared Decision-Making: Engaging in open discussions with the medical team about treatment options, weighing benefits and risks, and aligning care plans with personal values and goals.
Chapter 5: The Horizon and Beyond – Future Chapters in the CAD Story
The story of CAD is far from over. Medical science continues to write new chapters, pushing the boundaries of understanding and treatment.
- Genomic Medicine: Advanced genetic screening may one day precisely identify individuals at highest risk, allowing for hyper-personalized prevention strategies. Gene editing therapies could potentially correct underlying genetic predispositions.
- Artificial Intelligence and Big Data: AI is poised to revolutionize risk prediction, diagnostic imaging interpretation, and treatment optimization, allowing for earlier detection and more precise interventions.
- Novel Therapeutic Targets: Research is exploring new pathways beyond cholesterol and inflammation, such as targeting specific proteins involved in plaque formation, novel anti-inflammatory agents, or even regenerative medicine approaches to repair damaged heart tissue.
- Advanced Imaging: Non-invasive imaging techniques continue to evolve, offering clearer views of plaque characteristics and vulnerability, allowing for more accurate risk stratification.
- Precision Medicine: Moving away from a "one-size-fits-all" approach, future treatments will be increasingly tailored to an individual's unique genetic makeup, lifestyle, and disease profile.
- Social Determinants of Health: A growing understanding of how socioeconomic factors, access to healthy food, safe environments, and healthcare equity profoundly impact CAD prevalence and outcomes. Addressing these systemic issues is a critical future frontier.
Conclusion: The Enduring Power of Action and Hope
Coronary Artery Disease is a formidable antagonist in the human health narrative. It represents a complex interplay of biology, environment, and personal choices. Yet, this story is not one of inevitable decline, but of profound empowerment.
From the meticulous understanding of atherosclerosis to the strategic deployment of lifestyle modifications, pharmacological agents, and advanced interventions, humanity has amassed a powerful arsenal against this silent siege. The essential steps for prevention and management are clear: embrace a heart-healthy lifestyle, meticulously manage risk factors, adhere to prescribed medical therapies, and actively engage in shared decision-making with a dedicated healthcare team.
The story of CAD reminds us that our health is not a passive state but an active, ongoing endeavor. It is a narrative where knowledge becomes power, where discipline transforms into resilience, and where every conscious choice to nurture our hearts writes a chapter of vibrant, extended life. The fight against CAD is a collective effort, a continuous journey of scientific discovery and personal commitment, promising a future where the heart can beat stronger, longer, for all.